Our Health Library information does not replace the advice of a doctor. Please be advised that this information is made available to assist our patients to learn more about their health. Our providers may not see and/or treat all topics found herein.
Human Papillomavirus (HPV) Test of the Cervix
Test Overview
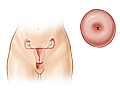
A human papillomavirus (HPV) test is done to check for a high-risk HPV infection. Like a Pap test, an HPV test is done on a sample of cells collected from the cervix. HPV is a sexually transmitted infection (STI). An HPV test checks for the genetic material (DNA) of the human papillomavirus.
This test is used to show whether a high-risk type of HPV is present. High-risk types of HPV (such as types 16, 18, 31, and 45) cause changes in the cells of the cervix that can be seen as abnormal changes on a Pap test. Abnormal cervical cell changes may get better on their own without treatment. But some cervical cell changes can progress to serious problems. They may lead to cervical cancer over time if they're not treated.
There are many types of HPV. Some low-risk types cause common skin warts. Some cause genital warts. These may be diagnosed during a physical exam. Other types don't cause any symptoms. Most people don't know they have an HPV infection.
Why It Is Done
An HPV test is done to check for high-risk types of human papillomavirus (HPV). High-risk types of HPV are linked to precancerous cervical cell changes and cervical cancer. If an HPV test shows that high-risk types of HPV are present, more testing (such as a colposcopy or cervical biopsy) may be recommended.
A Pap test or an HPV test can be used to screen for cervical cancer. An HPV test may be done at the same time as a Pap test or by itself. The results of an HPV test can help doctors decide if further tests or treatments are needed.
How To Prepare
Before an HPV test, you may be asked to not douche, use tampons, or use vaginal medicines for at least 24 hours.
You may be asked to empty your bladder just before the test, both for your own comfort and to help with the exam.
Talk to your doctor about any concerns you have regarding the need for the test, its risks, how it will be done, or what the results will mean.
How It Is Done
For this test, you need to remove your clothes below the waist and drape a paper or cloth covering around your waist. You will then lie on your back on an examination table with your knees bent and legs and feet supported by footrests. This allows your doctor to examine your vagina and vulva.
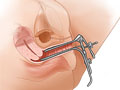
Your health professional will place an instrument called a speculum into your vagina. The speculum opens the vagina a little bit, allowing the inside of the vagina and the cervix to be examined.
Your health professional will then use a cotton swab or a small brush to collect several samples of cells from the cervix. Cells are collected from the visible part of the cervix as well as cells from inside the opening of the cervix (endocervical canal). The samples are then placed in collection tubes and sent to a laboratory for analysis.
How It Feels
You may feel some pressure or mild discomfort when the speculum is placed in your vagina. You may also feel some pressure when the sample of cervical cells is being collected.
Risks
There is very little chance of a problem from an HPV test.
Results
Normal: | High-risk HPV is not found. |
|---|---|
Abnormal: | High-risk HPV is found. If high-risk HPV is found, you may have a higher chance of having precancerous cervical cell changes. Further testing—including repeat Pap or HPV tests, colposcopy, or cervical biopsy—may be recommended by your doctor, depending on your medical history and the results of this test. |
A positive HPV test does not mean that you have cervical cancer. It may mean that you are infected with one or more high-risk types of HPV, which increases your chance of having precancerous cervical cell changes. Your doctor may recommend repeat testing or further testing, such as a colposcopy and cervical biopsy, to find out whether precancerous changes are present.
Related Information
Credits
Current as of: May 5, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: May 5, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use and Privacy Policy. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024-2025 Ignite Healthwise, LLC.