Our Health Library information does not replace the advice of a doctor. Please be advised that this information is made available to assist our patients to learn more about their health. Our providers may not see and/or treat all topics found herein.
Cold Temperature Exposure
It's easy to get cold quickly if you are outside in wet, windy, or cold weather. Cold temperature exposure can also happen if you spend time in a dwelling or other building that isn't well heated during cold weather.
Injuries from cold exposure
- "Frostnip" usually affects the skin on the face, ears, or fingertips. It may cause numbness or blue-white skin color for a short time. But normal feeling and color return quickly when you get warm. No permanent tissue damage occurs.
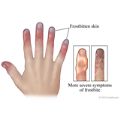
- Frostbite is freezing of the skin and the tissues under the skin because of temperatures below freezing. Frostbitten skin looks pale or blue. It feels cold, numb, and stiff or rubbery to the touch. With severe frostbite, you may have blisters. You can also get a skin injury by touching cold items such as dry ice without wearing gloves for protection.
- Cold injuries, such as trench foot and chilblains, may cause pale and blistered skin like frostbite after the skin has warmed. These injuries occur from spending too much time in temperatures that are cold, but not freezing. The skin doesn't actually freeze.
- Eye pain or vision changes caused by cold exposure most often occur in people who try to force their eyes open in high winds or cold weather, or during activities such as snowmobiling or cross-country skiing. Snow blindness is caused by sunlight reflecting off the snow and can cause a corneal injury or burn. Eyelids may become red and swollen. Eyes may feel dry and like they have sand in them.
- An abnormally low body temperature (hypothermia) occurs when the body loses heat faster than it can make heat. Symptoms include shivering, clumsy movements, confusion, poor judgment, and cold, pale, or blue-gray skin. Hypothermia is an emergency condition and needs medical care right away to stop heat loss.
Risk factors for cold exposure injury
There are many things that increase your risk of injury from exposure to cold temperatures. They include:
- Being a baby. A baby's body heat is lost faster when exposed to cold weather conditions.
- Being an older adult. Older people don't produce as much heat energy. And they may have health conditions that increase their risk.
- Drinking alcohol. Alcohol may affect your judgment. For example, a person may not put on more clothing when it's needed if their judgment is affected by alcohol.
- Being in outdoor conditions, such as high altitudes or wet and windy weather, and not being dressed properly.
- Having wet skin, wearing wet clothing, or being immersed in cold water.
- Being exposed to cold temperatures in your workplace, such as working in cold-storage units.
- Having certain health conditions, such as:
- Diabetes or cancer, or taking any medicines that may affect how you regulate your body temperature.
- Hypothyroidism or Raynaud's phenomenon that make you react more strongly to cold temperatures.
Many people get cold hands or feet. You're more likely to feel cold easily if:
- You don't have much body fat. Fat under the skin helps keep you warm. People who have low body fat may be more likely to get hypothermia. Babies, older adults, people with health conditions, and people who aren't getting enough food often have low body fat.
- You smoke cigarettes or drink caffeine. Nicotine (from tobacco) and caffeine cause narrowing of the blood vessels in the hands and feet. This causes less blood flow to these areas, so the hands and feet feel cold.
- You're under a lot of stress or feel tired. Chronic stress or anxiety can cause your nervous system to release adrenaline. It narrows the blood vessels that supply blood to the hands and feet.
Check Your Symptoms
The medical assessment of symptoms is based on the body parts you have.
- If you are transgender or nonbinary, choose the sex that matches the body parts (such as ovaries, testes, prostate, breasts, penis, or vagina) you now have in the area where you are having symptoms.
- If your symptoms aren’t related to those organs, you can choose the gender you identify with.
- If you have some organs of both sexes, you may need to go through this triage tool twice (once as "male" and once as "female"). This will make sure that the tool asks the right questions for you.
Many things can affect how your body responds to a symptom and what kind of care you may need. These include:
- Your age. Babies and older adults tend to get sicker quicker.
- Your overall health. If you have a condition such as diabetes, HIV, cancer, or heart disease, you may need to pay closer attention to certain symptoms and seek care sooner.
- Medicines you take. Certain medicines, such as blood thinners (anticoagulants), medicines that suppress the immune system like steroids or chemotherapy, herbal remedies, or supplements can cause symptoms or make them worse.
- Recent health events, such as surgery or injury. These kinds of events can cause symptoms afterwards or make them more serious.
- Your health habits and lifestyle, such as eating and exercise habits, smoking, alcohol or drug use, sexual history, and travel.
Try Home Treatment
You have answered all the questions. Based on your answers, you may be able to take care of this problem at home.
- Try home treatment to relieve the symptoms.
- Call your doctor if symptoms get worse or you have any concerns (for example, if symptoms are not getting better as you would expect). You may need care sooner.
Pain in adults and older children
- Severe pain (8 to 10): The pain is so bad that you can't stand it for more than a few hours, can't sleep, and can't do anything else except focus on the pain.
- Moderate pain (5 to 7): The pain is bad enough to disrupt your normal activities and your sleep, but you can tolerate it for hours or days. Moderate can also mean pain that comes and goes even if it's severe when it's there.
- Mild pain (1 to 4): You notice the pain, but it is not bad enough to disrupt your sleep or activities.
Pain in children under 3 years
It can be hard to tell how much pain a baby or toddler is in.
- Severe pain (8 to 10): The pain is so bad that the baby cannot sleep, cannot get comfortable, and cries constantly no matter what you do. The baby may kick, make fists, or grimace.
- Moderate pain (5 to 7): The baby is very fussy, clings to you a lot, and may have trouble sleeping but responds when you try to comfort him or her.
- Mild pain (1 to 4): The baby is a little fussy and clings to you a little but responds when you try to comfort him or her.
Early symptoms of hypothermia may include:
- Shivering.
- Cold, pale, or blue-gray skin.
- Clumsy movements.
- Poor judgment and a lack of interest in or concern about what's going on.
- Not speaking clearly.
Cold injury to the skin may cause:
- Severe pain.
- Numbness, tingling, or a prickly feeling.
- Hard, stiff, shiny, or rubbery skin.
- Cold, pale, white, pink-purple, or blue-gray skin.
- Blisters or sores.
Low body temperature means:
- In an adult or older child, 95 °F (35 °C) or lower.
- In a baby, 97 °F (36.1 °C) or lower. Rectal temperatures are the most accurate.
Some people's skin is very sensitive to cold temperatures and reacts abnormally. For example:
- The fingers, toes, nose, or ears may turn pale or white. Later they may turn blue.
- These areas may feel numb and tingly and feel very cold to the touch.
- As the areas warm, they may turn red and start to throb.
Symptoms of severe hypothermia may include:
- Stumbling and having trouble walking.
- Weakness, confusion, or extreme sleepiness.
- Slow, shallow breathing.
- Slow or uneven pulse.
- Passing out.
Call 911 Now
Based on your answers, you need emergency care.
Call 911 or other emergency services now.
Sometimes people don't want to call 911. They may think that their symptoms aren't serious or that they can just get someone else to drive them. Or they might be concerned about the cost. But based on your answers, the safest and quickest way for you to get the care you need is to call 911 for medical transport to the hospital.
Seek Care Now
Based on your answers, you may need care right away. The problem is likely to get worse without medical care.
- Call your doctor now to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or you don't have one, seek care in the next hour.
- You do not need to call an ambulance unless:
- You cannot travel safely either by driving yourself or by having someone else drive you.
- You are in an area where heavy traffic or other problems may slow you down.
Seek Care Today
Based on your answers, you may need care soon. The problem probably will not get better without medical care.
- Call your doctor or telehealth provider today to discuss the symptoms and arrange for care.
- If you cannot reach your doctor or telehealth provider or you don't have one, seek care today.
- If it is evening, watch the symptoms and seek care in the morning.
- If the symptoms get worse, seek care sooner.
What are your options for medical care?
Today your options for where to get your medical care are greater than ever before. You may not even have to leave your home to get the care you want and need. You can choose based on what your health problem is and what works best for you.
- Telehealth is a video call with a health care provider. It can be a convenient way to get medical advice or treatment. Some insurers provide access to telehealth that may be available 24 hours a day. Telehealth for less serious problems may cost less and be faster than in-person clinic visits.
- Urgent care and retail clinics are options if you don't have a doctor, you can't or don't want to wait to see your own doctor, or a telehealth visit can’t treat the problem.
- Virtual care from your primary provider or a telehealth service can be delivered through your smartphone, computer, or tablet.
Make an Appointment
Based on your answers, the problem may not improve without medical care.
- Make an appointment to see your doctor in the next 1 to 2 weeks, or contact your telehealth provider.
- If appropriate, try home treatment while you are waiting for the appointment.
- If symptoms get worse or you have any concerns, call your doctor or telehealth provider. You may need care sooner.
What are your options for medical care?
Today your options for where to get your medical care are greater than ever before. You may not even have to leave your home to get the care you want and need. You can choose based on what your health problem is and what works best for you.
- Telehealth is a video call with a health care provider. It can be a convenient way to get medical advice or treatment. Some insurers provide access to telehealth that may be available 24 hours a day. Telehealth for less serious problems may cost less and be faster than in-person clinic visits.
- Urgent care and retail clinics are options if you don't have a doctor, you can't or don't want to wait to see your own doctor, or a telehealth visit can’t treat the problem.
- Virtual care from your primary provider or a telehealth service can be delivered through your smartphone, computer, or tablet.
Self-Care
When you are exposed to the cold, first aid measures may prevent further heat loss and help the body slowly warm up. Try these ideas.
- Stay calm. Fear or too much activity causes sweating. Sweating can make you feel chilled.
- Find shelter. Get out of the cold, the wind, or the water.
- Remove cold, wet clothes.
- Put on dry clothing—made of moisture-wicking fabrics, such as wool, polyester, or nylon (not cotton)—that insulates well. Cover your head.
- If dry clothing is not immediately available, you can try to get warm by making skin-to-skin contact. After removing wet clothes, wrap a blanket or sleeping bag around you and another person and allow body heat to rewarm you.
- Warm up under a heated blanket, if available.
- Move around, but don't be so active that you sweat. Whirl your arms around like a windmill to get your blood moving and warm you up. Activity makes body heat and improves blood flow. Sweating should be avoided because it cools the body.
- Drink warm fluids and eat. Avoid drinks with caffeine or alcohol. Eat high-energy foods, such as candy. Do not give food or drink to a person who is acting confused or responding slowly.
- Do not use a warm water bath to try to warm up. Taking a warm water bath may cause more problems. Continue to try other methods, and monitor closely.
- Do not use tobacco.
- Be careful with heaters and fires so you don't get burned. Be aware that if you (or the person) sit in front of a heater or a fire to warm up, there is a greater chance of getting burned. This is because normal feeling is lost in cold-injured skin, and you may not know when to move away from the heater or fire.
- Protect your skin. Frostbitten skin may be more sensitive after the cold injury. The injured skin area should be protected with sunscreen and protective clothing to prevent further skin damage. The color of the injured skin may also change over time.
When to call for help during self-care
Contact a doctor if any of the following occur during self-care at home:
- New or worse blisters.
- New or worse symptoms of infection, such as redness, warmth, swelling, pus, or a fever.
- Symptoms that occur more often or are more severe.
Learn more
Preparing For Your Appointment
Related Information
Credits
Current as of: October 1, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: October 1, 2025
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Ignite Healthwise, LLC education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use and Privacy Policy. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024-2026 Ignite Healthwise, LLC.